Prior authorizations are a standard operating procedure across almost all insurance plans. Not all medical events need prior authorizations, but several interventions, such as procedures not typically covered by a health plan, expensive drugs or medical techniques, methods or pharmaceuticals that are limited in their approved uses, or drugs prescribed at a unique dosage will all require one before being covered by insurance plans.
Prior authorizations protect insurance companies against superfluous, fraudulent, or redundant medical interventions while maintaining quality care for those seeking treatment.
Prior authorization, however, as the name suggests, must be completed before any treatment is executed. In 2021, the CAQH Index reported Payers could save 16 minutes of processing time for medical prior authorizations by moving from manual processing to automated processing. While saving time in minutes doesn’t seem like much on its own, it becomes a tremendous volume when compounded over millions of authorizations.
Table of Contents
Automation Trends in Medical Prior Authorizations
Automating medical prior authorizations is gaining steam, but there’s plenty of room for growth and monetary incentives with increased automation. The CAQH estimates that nearly a half-billion dollars could be saved annually by moving prior authorizations to automated systems.
The benefits of automating authorizations extend beyond monetary. Gartner reported that physicians can find prior authorizations “burdensome,” and with physician burnout increasing, looking for ways to reduce these administrative tasks is crucial to enhancing retention.
Delaying insurance pre-authorizations has also been linked to adverse outcomes for patients. Decisions stemming from prior authorization details on whether patients are allowed to be treated, or treated in a certain way, can impact the quality and timing of the treatment they receive altogether. This is where an extra 16 minutes per claim with manual processing really comes into play.
Barriers to Automating Medical Prior Authorizations
Several hurdles stand in the way of authorization automation. By nature, these authorizations are complex, requiring a thoughtful discernment of the data that’s being transferred. Similarly, laws vary from state to state, adding another layer that needs to be determined before giving the all-clear. Because of these barriers, among others, the digital infrastructure simply hasn’t been built to handle automated pre-auths quickly and efficiently, which in itself adds to the impediments of moving from manual to automated processing.
How to Make Meaningful Steps Forward with Automation
A trusted healthcare technology partner can help. Because of the unique nature of prior authorizations and their nuanced characteristics, there will never be a universal out-of-the-box solution. Smart Data Solutions (SDS) has more than 80 in-house technologists who can work with Provider and Payer teams to help optimize their workflows.
Starting strategically with a portion of the work and incrementally adding automation to increase efficiency over time is the best approach to deal with such nuanced information. This methodical approach to automation ensures:
- The systems work as intended
- Data is properly captured or transferred and ultimately results in minimal errors
- Human intervention can be reduced
SDS also looks to move away from legacy systems and toward the CAQH CORE Prior Authorization & Referrals Operating Rules: X12 278 by using intelligent automation to create efficiencies.
“These operating rule requirements reduce the unnecessary back and forth between providers and health plans, accelerate adjudication timeframes and reduce provider resources spent on manual follow up. “ – CAQH
How SDS Automates the Medical Prior Authorization Process
Smart Data Solutions has 20+ years of healthcare IT experience helping companies automate processes. Our prior authorization process typically follows the below steps:
- Document classification and workflow routing.
- Identify Member and Patient. Identify Provider and determine Par vs. Non-Par.
- Determine services rendered. Review and analyze medical record data and attachments.
- Recommend authorization through predictive decision support.
- Automate authorization.
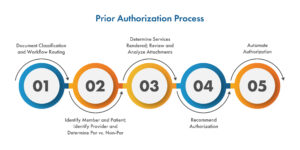
These steps can vary based on the current in-house technology or immediate needs to deliver benefits quickly. Outcomes include faster and more accurate prior authorization decisions and an increase in throughput while reducing backlog.
Automating prior authorizations only brings benefits to Payers and Providers alike. Reduced workload on staff and greater allocation of human capital, potentially better patient outcomes, and reduced frustration among physicians and administrators.
If you’re interested in learning about how intelligent automation can alleviate headaches with medical prior authorizations, then connect with us today. We’ll show you how our in-house technologists craft custom solutions to take the manual burden out of prior authorization processing.
